Have you recently had one or more teeth extracted? Do you feel a deep pain at the extraction site? Are you experiencing tooth sensitivity when you eat or drink anything cold, hot, or sweet? If you answered yes to any of these questions, then you might have a dry socket. A dry socket is the most common complication that occurs after a tooth extraction. Although dry sockets don’t affect every individual who has an extraction, if you have one you will definitely want to know more about it. Here is everything you need to know about a dry socket:
What It Is
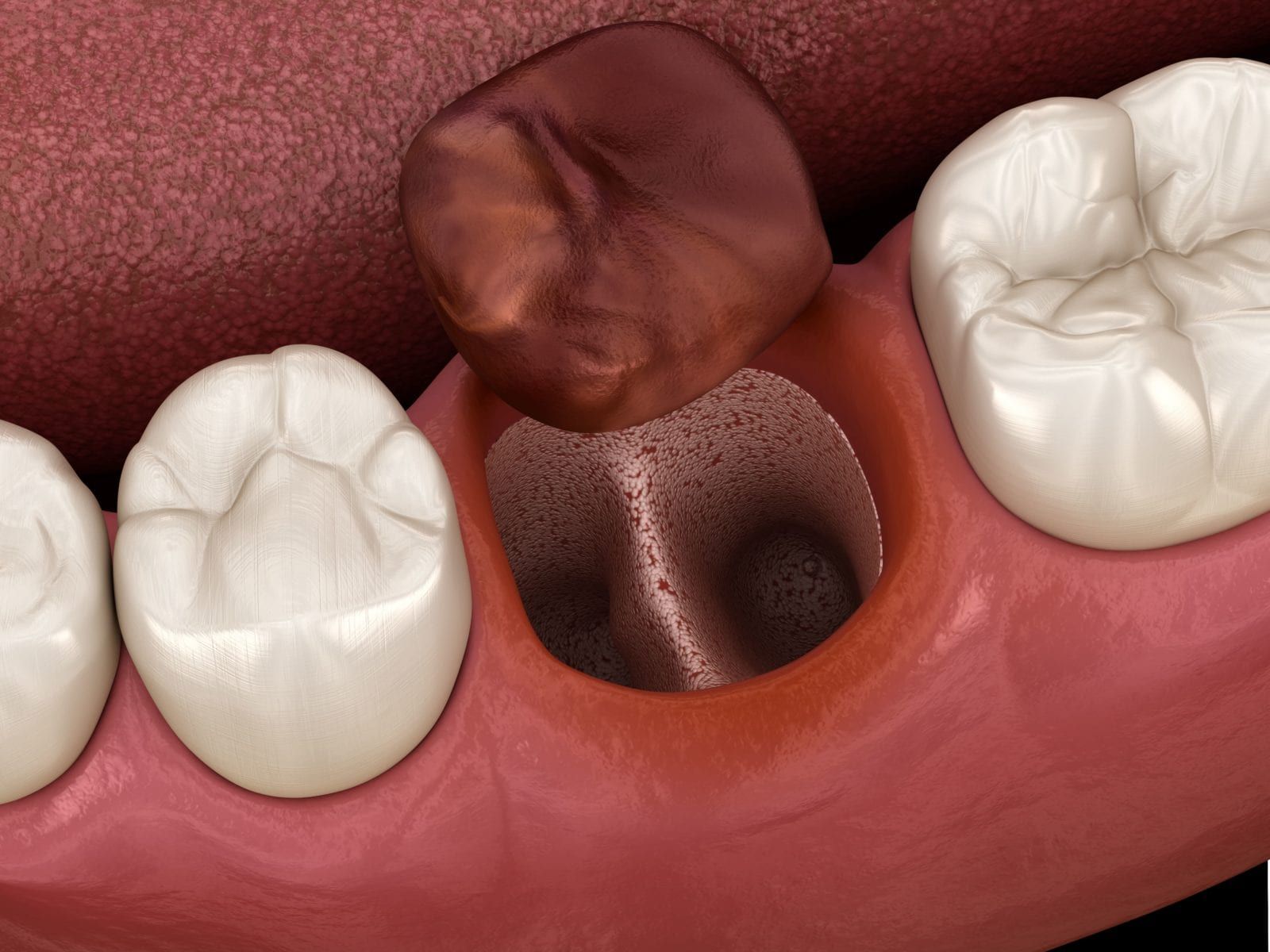
The scientific name for a dry socket is alveolar osteitis, which literally means inflammation of the alveolar bone. It occurs when the body fails to form a protective blood clot at the extraction site or when this blood clot is dislodged. This leaves the alveolar bone exposed, as well as raw tissue and nerve endings. Although a dry socket can occur after any tooth is extracted, they are more likely to occur in molars and teeth in the lower jaw.
Do You Have a Dry Socket?
As mentioned above, a dry socket leaves the bone, tissue, and nerve endings exposed. This unfortunately means that one of the primary symptoms associated with dry sockets are pain. Specifically, pain caused by a dry socket is characterized as a deep, throbbing pain on the side of the extraction. In some cases, this pain may be severe and/or it may radiate through the entire side of your face. Other signs of a dry socket include a bad taste and smell in your mouth. Additionally, if you are able to see exposed bone when you look at the socket, this likely means you have a dry socket.
What to do if You Think You Have a Dry Socket
If you think you may have a dry socket, the first thing you should do is call your dentist to report your symptoms and request an appointment. Extreme pain after a tooth extraction is not normal and you don’t need to tough it out. At your appointment, your dentist will examine the extraction site to determine if a dry socket is present or if there are any signs of infection. Next, they will clean the socket by flushing out any debris that may have accumulated within it. A pain relieving medication will be placed in the socket and the socket will be packed with gauze to keep the medication in place. Once the socket has been packed, the pain will usually subside rather quickly. In some cases, your dentist may provide you with materials and instructions on how to pack the socket at home.
Can Dry Sockets be Prevented?

There are some cases where you may be able to prevent a dry socket from occurring in the first place. For starters, some individuals may be at an increased risk of developing a dry socket and should take preventative measures. You may be at an increased risk of developing a dry socket if you have had one in the past, smoke or use tobacco products, or are on oral contraceptives.
While there is nothing that can be done if your body fails to make a protective clot, you can take preventative measures to avoid disloding the protective blood clot. Here are a few things you can do to reduce the risk of developing a dry socket:
- Avoid vigorous activity that can dislodge the clot
- Don’t drink from a straw (suction can dislodge the clot)
- Don’t smoke (suction can dislodge the clot and tobacco delays healing)

Dr. Mark and Dr. Gina Covington are committed to providing their patients with the highest level of care. Both doctors are members of the Academy of General Dentistry as well as the American Dental Association. Locally, both belong to the Western Piedmont Dental society and the Foothills Dental Continuum. Because dentistry is a dynamic field, continued education is a paramount concern. Both Dr. Mark and Dr. Gina have completed several hundred hours of continued education to become proficient in the science and placement of dental implants. This course of study has allowed them to become Fellows of the International Congress of Oral Implantologists.


